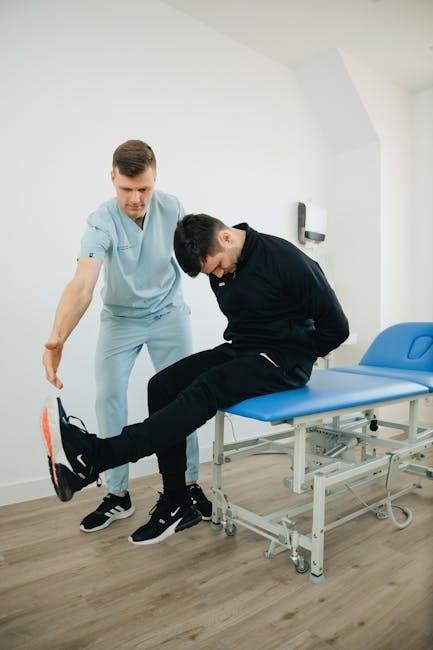
Physical therapy documentation is crucial for patient care‚ legal protection‚ and reimbursement; PDF formats are frequently utilized for their accessibility and preservation qualities.
Software solutions‚ like EHR systems‚ streamline this process‚ enhancing record management and patient outcomes‚ especially with musculoskeletal disease prevalence increasing.
Value-based reimbursement and outcome measures further emphasize the need for detailed‚ accurate records‚ often delivered as PDF reports.
The Critical Role of Accurate Documentation
Accurate physical therapy documentation isn’t merely a clerical task; it’s the cornerstone of responsible patient care and professional liability protection. Detailed records‚ often compiled and shared as PDF documents‚ provide a clear timeline of a patient’s condition‚ interventions‚ and progress – or lack thereof. This meticulous record-keeping is vital for effective communication between therapists‚ physicians‚ and other healthcare providers‚ ensuring continuity of care.
Furthermore‚ precise documentation directly impacts reimbursement claims. Insurance companies require comprehensive evidence to justify the necessity and effectiveness of treatments. PDF documentation serves as that evidence‚ supporting billing accuracy and minimizing claim denials. The increasing focus on value-based reimbursement models makes this even more critical‚ demanding demonstrable outcomes.
Beyond financial considerations‚ robust documentation significantly reduces legal risks. In the event of a dispute or legal challenge‚ well-maintained records – frequently distributed as PDF files – offer a strong defense‚ demonstrating adherence to professional standards and appropriate care. Software solutions designed for physical therapy streamline this process‚ enhancing record management and minimizing potential errors.
Why PDF Format is Common for Documentation
PDF (Portable Document Format) has become a ubiquitous standard in physical therapy documentation due to its inherent advantages. Primarily‚ PDFs preserve document formatting across different operating systems and devices‚ ensuring consistent presentation regardless of the recipient’s software. This is crucial for legal and clinical accuracy when sharing physical therapy documentation examples.
PDFs also offer enhanced security features‚ allowing for password protection and restricted editing‚ safeguarding sensitive patient information – a critical aspect of HIPAA compliance. Their compact file size facilitates easy storage and efficient transmission via email or secure portals.
Many EHR (Electronic Health Record) systems readily generate reports in PDF format‚ streamlining the documentation process. The format’s universality and reliability make it ideal for archiving and long-term record retention‚ ensuring accessibility for future reference and potential legal reviews. This widespread compatibility solidifies PDF’s position as the preferred choice.
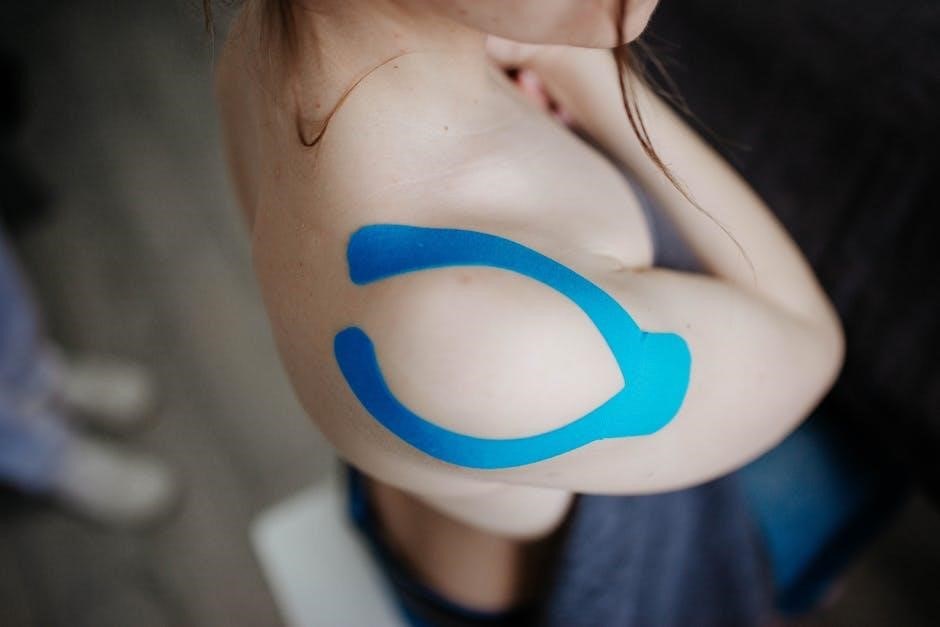
Essential Components of Physical Therapy Notes
Physical therapy notes require Subjective‚ Objective‚ Assessment‚ and Plan sections (SOAP); PDF examples demonstrate comprehensive patient care documentation.
Accurate records are vital for legal protection and effective treatment tracking.
Subjective Examination (S-Section)
The Subjective (S) section of physical therapy notes meticulously documents the patient’s perspective‚ forming a cornerstone of comprehensive care. PDF documentation examples highlight the importance of capturing the patient’s chief complaint in their own words‚ detailing the history of their present illness‚ and outlining any relevant past medical history.
This section isn’t merely a recitation of symptoms; it’s a narrative built upon Patient Reported Outcomes (PROs). These PROs‚ often captured through standardized questionnaires‚ provide quantifiable data regarding pain levels‚ functional limitations‚ and overall quality of life.
Effective documentation includes social history factors impacting recovery‚ such as work demands‚ lifestyle‚ and psychological factors. A well-crafted S-section‚ often presented within a PDF report‚ establishes a clear understanding of the patient’s experience‚ guiding subsequent objective assessments and treatment planning. Accurate and detailed subjective reporting is paramount for effective patient-centered care.
Patient Reported Outcomes (PROs) in Documentation
Patient Reported Outcomes (PROs) are integral to modern physical therapy‚ and their inclusion in PDF documentation demonstrates a commitment to patient-centered care. These standardized measures quantify a patient’s functional status‚ pain levels‚ and perceived disability‚ offering valuable insights beyond traditional clinical assessments;
PDF examples showcase various PRO instruments‚ such as the Numeric Pain Rating Scale‚ the Oswestry Disability Index (for low back pain)‚ or the DASH (Disabilities of the Arm‚ Shoulder and Hand) questionnaire. Documenting the score itself is insufficient; clinicians must also note the patient’s interpretation of the score and how it relates to their daily life.
Trends in PRO scores‚ tracked over time within PDF progress notes‚ provide objective evidence of treatment effectiveness. Utilizing PROs strengthens clinical reasoning‚ supports billing justifications‚ and ultimately enhances the quality of care delivered.
Objective Examination (O-Section)
The Objective (O) section of physical therapy notes‚ frequently detailed in PDF format‚ meticulously records measurable data gathered during the examination. This includes vital signs‚ posture analysis‚ range of motion (ROM) measurements‚ muscle strength testing‚ neurological assessments‚ and special tests.
PDF documentation examples demonstrate precise recording of ROM using goniometry‚ specifying joint angles and movement quality. Manual Muscle Testing (MMT) results are documented using the standard grading scale (0-5). Objective findings must be factual and avoid subjective interpretations; for instance‚ instead of “weakness‚” document “MMT 4/5.”
Clear‚ concise language within the PDF ensures accurate communication among healthcare professionals. The O-section forms the foundation for the assessment‚ justifying the chosen treatment plan and demonstrating the therapist’s clinical expertise.
Goniometric Measurements & Recording
Goniometry‚ a cornerstone of objective assessment‚ precisely measures joint range of motion (ROM). PDF documentation examples showcase standardized recording: joint‚ motion‚ starting and ending angles‚ and any limitations or pain. Active and passive ROM are documented separately‚ noting any discrepancies.
Accuracy is paramount; therapists must correctly identify bony landmarks and align the goniometer’s axis with the joint’s axis of motion. PDF reports should clearly indicate the type of goniometer used (universal‚ inclinometer). Documenting muscle length tests alongside goniometry provides a comprehensive picture.
Consistent recording within PDF notes allows for reliable tracking of progress; Documenting deviations from normal values and any associated symptoms is crucial for informed clinical decision-making and effective treatment planning.
Manual Muscle Testing (MMT) Documentation
Manual Muscle Testing (MMT) assesses muscle strength‚ a vital component of the objective exam. PDF documentation examples demonstrate clear recording using the standard grading scale (0-5)‚ detailing the muscle group tested and the grade achieved. Precise notation is key; for example‚ “Hip Flexors: 4/5‚ with fatigue.”
Documenting the testing position‚ resistance level‚ and any pain experienced during testing is essential. PDF reports should also note any compensatory movements observed. If a muscle tests below 4/5‚ further investigation and documentation of contributing factors are necessary.
Consistent MMT documentation within PDF notes enables tracking strength gains or declines. This data informs treatment progression and demonstrates the effectiveness of interventions‚ supporting value-based care initiatives.

Assessment (A-Section) – Interpreting Findings
Assessment in PDF documentation synthesizes subjective and objective data‚ forming a problem list and justifying the clinical reasoning behind the chosen treatment plan.
Problem List Creation & Prioritization
Creating a comprehensive problem list‚ often documented within a PDF report generated from EHR systems‚ is fundamental to effective physical therapy. This list should clearly articulate each patient impairment‚ functional limitation‚ and disability identified during the examination process.
Prioritization is equally vital; problems should be ranked based on their impact on the patient’s functional abilities and their potential to respond to intervention. This prioritization guides treatment planning and ensures that the most significant issues are addressed first.
A well-structured problem list‚ frequently included in initial evaluations and progress notes as PDF attachments‚ demonstrates clinical reasoning and supports appropriate billing and reimbursement. Accurate documentation‚ especially regarding musculoskeletal conditions‚ is crucial for value-based care and outcome measurement‚ as highlighted by recent market trends.
The problem list should be dynamic‚ updated with each encounter to reflect the patient’s progress and any new concerns that arise‚ ensuring the PDF documentation remains a current and accurate representation of their condition.
Clinical Reasoning & Justification
Clinical reasoning is the cornerstone of effective physical therapy‚ and its clear documentation – often within a PDF generated from an EHR – is paramount. This involves articulating the thought process behind assessment findings and treatment decisions‚ demonstrating a logical connection between evaluation results and the chosen interventions.
Justification for each intervention must be explicitly stated‚ referencing evidence-based practice and explaining how the treatment addresses the identified problems. This detailed rationale strengthens the PDF documentation and supports claims for reimbursement‚ particularly within value-based care models.
Proper documentation‚ as emphasized by resources on liability reduction‚ protects the practitioner and ensures continuity of care. A well-reasoned PDF report‚ detailing the therapist’s clinical judgment‚ is essential when managing musculoskeletal conditions and tracking patient outcomes.
The ability to clearly articulate clinical reasoning enhances professional credibility and demonstrates a commitment to providing high-quality‚ patient-centered care‚ all readily accessible within the PDF format.

Plan (P-Section) – Treatment Strategies
Treatment plans‚ often detailed in PDF reports from EHR systems‚ outline specific techniques and a Home Exercise Program (HEP) for optimal patient recovery.
These strategies are crucial for managing musculoskeletal issues and achieving measurable outcomes.
Treatment Techniques Documented
Detailed documentation of treatment techniques is paramount within the P-section‚ frequently presented in PDF format generated from EHR systems. This includes specifics like therapeutic exercise – specifying sets‚ repetitions‚ resistance‚ and the patient’s response.
Manual therapy interventions‚ such as joint mobilization or soft tissue mobilization‚ require precise recording of grades‚ duration‚ and observed changes. Modalities utilized‚ like ultrasound or electrical stimulation‚ must include parameters (frequency‚ intensity‚ duration) and the rationale for their application.
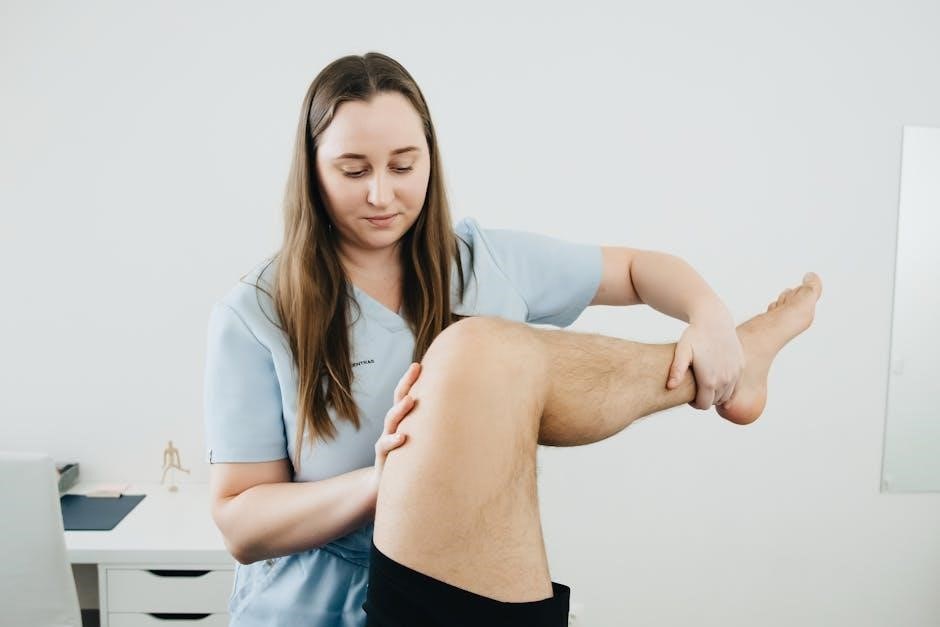
Functional training activities should be described with clarity‚ outlining the specific exercises and progressions used to address identified impairments. Accurate documentation supports clinical reasoning‚ justifies treatment choices‚ and facilitates continuity of care‚ especially when shared as a PDF report.

Furthermore‚ it’s vital to note patient tolerance and any adverse reactions to the techniques employed‚ ensuring a comprehensive and legally sound record.
Home Exercise Program (HEP) Instructions
HEP instructions‚ often delivered as a patient-friendly PDF‚ are a critical component of the P-section‚ promoting patient engagement and adherence. Documentation must detail each exercise‚ including clear descriptions‚ illustrations (if available)‚ sets‚ repetitions‚ frequency‚ and intensity levels.
Specific instructions regarding proper form and precautions are essential to minimize risk and maximize effectiveness. The rationale for each exercise‚ linking it back to the patient’s impairments and goals‚ enhances understanding and motivation.
EHR systems often facilitate PDF generation of customized HEPs‚ ensuring consistency and accuracy. Documenting patient education regarding the HEP‚ including their understanding and any barriers to adherence‚ is vital.
Progressive overload strategies should be outlined‚ guiding patients on how to safely advance their exercises over time‚ contributing to improved outcomes and a well-documented care plan.

Specific Documentation Examples
PDF examples of initial evaluations and progress notes demonstrate comprehensive documentation‚ showcasing subjective findings‚ objective measures‚ assessments‚ and detailed treatment plans.
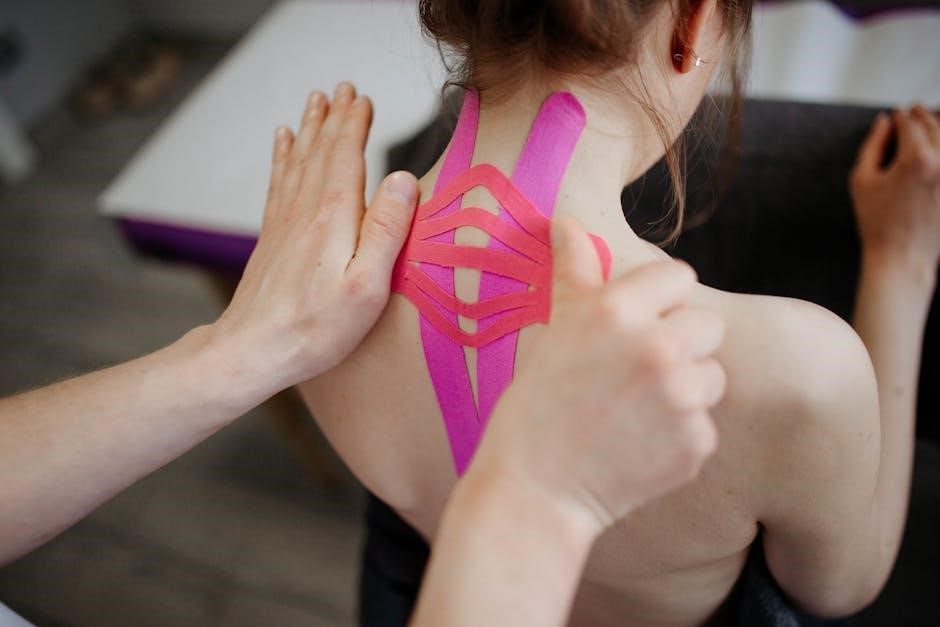
These PDFs illustrate how EHR systems facilitate accurate record-keeping‚ supporting legal compliance and optimal patient care.
Initial Evaluation Documentation Example
A comprehensive initial evaluation‚ often saved as a PDF‚ begins with detailed patient demographics and referral information. The Subjective section meticulously documents the patient’s history‚ including the onset of the current problem‚ prior medical history‚ and functional limitations reported by the patient themselves – utilizing Patient Reported Outcomes (PROs) where applicable.
The Objective section‚ also detailed in the PDF‚ presents measurable data; This includes Goniometric Measurements documenting range of motion‚ Manual Muscle Testing (MMT) results‚ postural assessments‚ neurological screenings‚ and special tests. All findings are clearly recorded with specific values and observations.
Crucially‚ the PDF will contain a clear problem list‚ identifying impairments and functional limitations. This initial evaluation‚ formatted as a PDF‚ serves as the baseline for tracking progress and justifying the treatment plan‚ ensuring accurate and legally sound documentation.
Progress Note Documentation Example
Progress notes‚ frequently generated as a PDF‚ detail the patient’s response to treatment over time. Each note begins with a concise Subjective update‚ summarizing the patient’s current symptoms and any changes since the last session. This section reflects ongoing Patient Reported Outcomes (PROs).
The Objective portion of the PDF documents measurable changes. This includes re-assessment of Goniometric Measurements and Manual Muscle Testing (MMT)‚ comparing results to the initial evaluation. Treatment techniques administered during the session are clearly outlined‚ along with dosage and patient tolerance.
The PDF also includes a brief Assessment section‚ interpreting the findings and adjusting the plan accordingly. Finally‚ the updated Plan details the next steps‚ including continued treatment and any modifications to the Home Exercise Program (HEP) instructions.

Legal and Ethical Considerations
Physical therapy documentation‚ often in PDF format‚ must adhere to HIPAA regulations‚ safeguarding patient privacy and minimizing potential liability risks for practitioners.
Accurate records are vital for legal defense and demonstrate responsible patient care.
HIPAA Compliance in Physical Therapy Documentation
Maintaining HIPAA compliance within physical therapy documentation‚ frequently utilizing PDF formats for record-keeping‚ is paramount. This involves stringent adherence to privacy rules regarding Protected Health Information (PHI).
PDF documents must be securely stored and accessed‚ employing encryption and access controls to prevent unauthorized disclosure. Documentation software‚ including EHR systems generating PDF reports‚ should be HIPAA-compliant‚ offering audit trails and data security features.
Practitioners must receive thorough training on HIPAA regulations and documentation best practices. Proper de-identification techniques are crucial when sharing data for research or quality improvement purposes. Failure to comply can result in significant penalties‚ emphasizing the importance of meticulous record management and secure PDF handling.
Regularly reviewing and updating security protocols is essential to adapt to evolving HIPAA guidelines and protect patient confidentiality.
Documentation & Liability Reduction
Comprehensive physical therapy documentation‚ often delivered as secure PDF reports‚ is a cornerstone of liability reduction for practitioners. Accurate and detailed records demonstrate the standard of care provided‚ justifying treatment decisions and outcomes.
PDF documentation should clearly outline patient history‚ examination findings‚ assessment‚ plan‚ interventions‚ and patient progress. Consistent and objective language minimizes ambiguity and potential misinterpretation. Utilizing EHR systems to generate these PDFs ensures a clear audit trail.
Proper documentation serves as legal evidence in the event of a dispute or claim. Software solutions designed for healthcare‚ as highlighted by SFGate.com‚ can significantly limit liability. Thorough documentation reflects professional competence and a commitment to patient safety‚ proactively mitigating risk.
Regular documentation audits are recommended to ensure completeness and accuracy.

Software Solutions for Physical Therapy Documentation
EHR systems revolutionize documentation‚ enabling efficient creation and management of PDF reports; they enhance record keeping and improve patient care workflows significantly.
These tools streamline processes‚ supporting value-based reimbursement and outcome measurement‚ crucial for modern physical therapy practice.
Benefits of Electronic Health Records (EHR)
Electronic Health Records (EHR) offer substantial advantages over traditional paper-based systems for physical therapy documentation‚ particularly regarding the creation and management of PDF reports.
EHRs improve accuracy and legibility‚ reducing errors and enhancing communication among healthcare professionals. They facilitate efficient data retrieval‚ enabling quicker access to patient history and treatment progress‚ which is vital for informed decision-making.
Furthermore‚ EHRs streamline billing and coding processes‚ minimizing claim denials and maximizing reimbursement. They support compliance with regulatory requirements‚ such as HIPAA‚ by providing robust security features and audit trails.
The ability to generate standardized PDF documentation ensures consistency and facilitates seamless sharing of information with other providers and insurance companies. This ultimately leads to better patient care and improved practice efficiency‚ especially with the increasing focus on value-based care and outcome measures.
EHRs also contribute to reduced administrative burden‚ allowing therapists to dedicate more time to direct patient care.
PDF Generation from EHR Systems
EHR systems excel in generating professional‚ compliant PDF documents for physical therapy notes‚ evaluations‚ and progress reports. This functionality is critical for secure data exchange and archiving.
Modern EHRs allow therapists to customize PDF templates‚ incorporating practice logos‚ standardized formatting‚ and required signatures. Automated features populate these templates with patient data‚ minimizing manual entry and reducing errors.
The generated PDFs are easily shareable via secure email‚ patient portals‚ or direct upload to insurance portals‚ streamlining communication and claim submissions. They also provide a reliable‚ long-term storage solution for patient records.
Furthermore‚ PDF generation from EHRs supports compliance with legal and ethical standards‚ including HIPAA regulations‚ by ensuring data integrity and confidentiality. This capability is increasingly important given the emphasis on value-based reimbursement and outcome measurement‚ requiring detailed documentation.
Efficient PDF creation enhances practice workflow and improves overall record management.